Real Wellbeing is being in balance
Sometimes life can feel overwhelming, a constant juggling act. We believe that being in balance is key to Real Wellbeing. Explore tips and research that will help you find balance and achieve Real Wellbeing.
What is Real Wellbeing?
Life is a constant juggling act
Finding balance is no easy task. Real Wellbeing relies on a range of factors that bring balance and satisfaction to your life.

The secret to a balanced life

From finances to future wishes: navigating financial and estate planning with ageing parents

Navigating new roles and difficult conversations for the sandwich generation
The latest tips, tools and stories
Health
Healthier lives from the inside out, top to toe
Ready to make some changes but don’t know where to start? Find some inspiration to improve your physical and mental health.

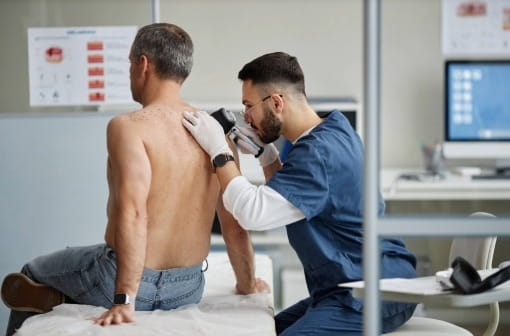
Regular skin checks: why early detection is vital to your wellbeing

The surprising link between gut health and mental wellbeing

Maximising your extras and wellbeing
The latest tips, tools and stories
Money & finances
Financial wellbeing for every stage and change
Saving? Budgeting? Investing? Find out what financial wellbeing could look like for you.

Women’s financial wellbeing: creating a financially equitable future

Financial inclusion: a building block of wellbeing

Stretch your budget and boost wellbeing with Wellplan Rewards
The latest tips, tools and stories
Goals & planning
Plan for the best (and the worst)
Whether you’re ticking off the big things or just getting your life in balance, we’ve got tips and tricks to help.

Your pregnancy tests and appointments

The important admin every new parent must know

Four steps to prepare for a natural hazard
The latest tips, tools and stories
Community & relationships
The people & places that make us who we are
Having a network to share our success with or support us in tough times is critical for wellbeing, so it’s important to keep those ties strong!

How to foster community connections for your wellbeing

Young and old: Why kids need older people in their lives