"They feel that they are valued. They know that when they bring something up, someone's listening."—Leona Macdonald, Home Care Services Branch Manager, Australian Unity
Key points
- An aging population is driving a rapidly growing demand for carers, with the Australian Government's Intergenerational Report indicating that the care workforce may need to double by 2049–50.
- The Australian Unity Wellbeing Index has shown that professional carers have wellbeing that sits at the top of the average range. In comparison, informal carers had lower wellbeing and higher mental distress.
- The Wellbeing Index also highlighted the importance of carer supports such as access to training and psychological support, and connection with other carers.
Australia’s population is aging fast. This year, the Australian Government's Intergenerational Report reported that the number of people aged 65 and over will more than double over the next 40 years, while the number aged 85 and over will more than triple. The result? An increasing demand that's set to fall on the nation’s carers.
In 2020–21, around 460,000 Australians worked as professional carers. But that number is woefully inadequate for what lies ahead. The Intergenerational Report suggests that in order to meet surging demand, the care workforce in 2049–50 may need to be twice the size it was in 2020–21.
“Professional carers are fundamental to the health of an aging population,” insists Prue Bowden, CEO of Home Health for Australian Unity.
"It's the human connection they bring to that activity," she says, pointing to the vital work carers do to monitor their customers' health and identify changing needs for support and services. "It's incredibly important that there are trusted people who are providing that social, emotional and physical care."
On a macro level, meanwhile, carers help to take the burden off the healthcare system. “We would have many more aged-care customers blocking beds in hospitals if we didn't have professional carers delivering quality care in the community,” says Prue.

Comparing carers' wellbeing
Carers are critical for our society, but the role can be challenging and is often undervalued. This year's Australian Unity Wellbeing Index—a 22-year study into the wellbeing of Australians, conducted in partnership with Deakin University—showed that professional carers had personal wellbeing scores that sat at the top of the average range.
By contrast, informal (unpaid) carers fared decidedly less well. “That group had a pattern of lower personal wellbeing scores and higher rates of mental distress, particularly those with large time commitments for caring” says lead researcher Dr Kate Lycett, from Deakin University’s School of Psychology.
Prue isn’t surprised by the fact that professional carers tend to fare better than their informal counterparts, pointing to the vocational aspect of the job for many people, as well as the benefits of training and support, connections with colleagues and, of course, remuneration for their efforts.
“When you think about the elements of Real Wellbeing, it's about social connection, a sense of achievement, security, and safety," says Prue. "Professional carers have the skills to be able to do their job effectively, so they feel safer in the delivery of that care. Having purpose in the profession you've chosen can also mean that you're more likely to get a sense of achievement and joy from your work.”
Sign up for wellbeing news
Get real wellbeing news, information and tips straight to your inbox.
The power of support
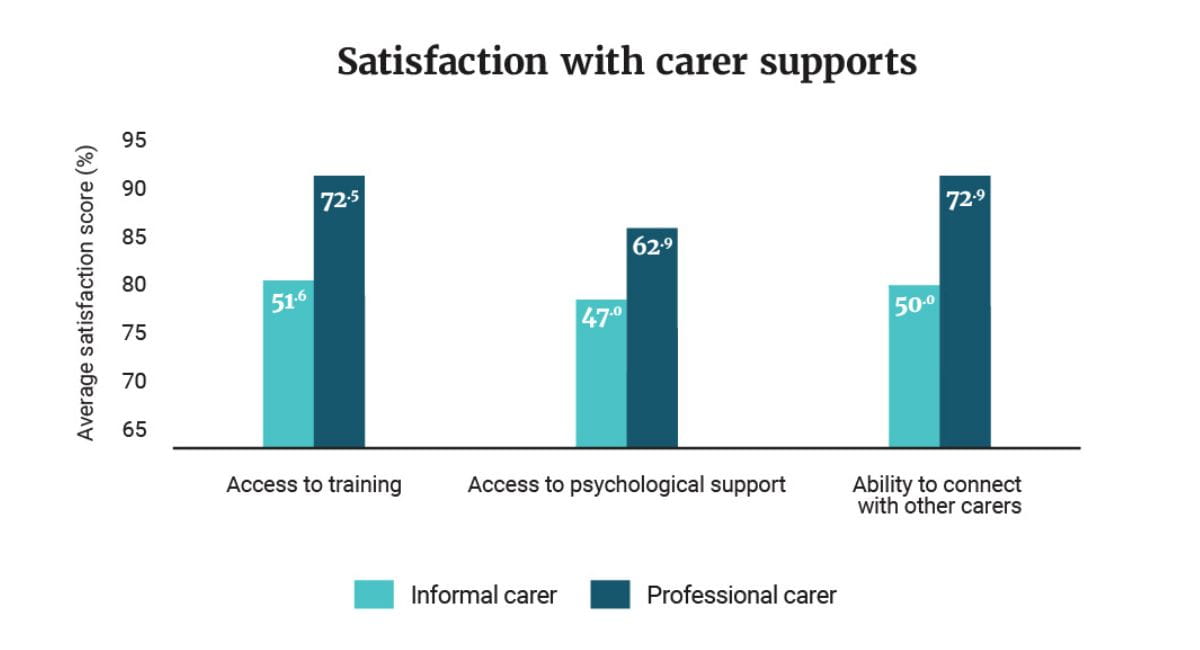
Prue’s insight is reinforced by this year’s Wellbeing Index, which explored how satisfied carers were with their access to training and skills courses, access to psychological support and ability to connect with other carers.
“There was a big difference in terms of their levels of satisfaction with access to these supports,” says Kate, highlighting that professional carers were far more satisfied across these areas than informal carers.
It's a finding that points to an important opportunity for care organisations as they seek to attract and retain skilled employees.
Creating carer supports
But what does this look like in a practical sense? As Leona Macdonald, Home Care Services Branch Manager for Australian Unity, knows firsthand the benefit that structured support and training can provide. "They feel that they are valued," she says of her team. "They know that when they bring something up, someone's listening.
Established guidelines and ongoing training—both in-person and online—help Australian Unity's carers to feel more confident in their roles, while regular catch-ups, team meetings and one-on-ones with coaches also present opportunities to seek advice or simply vent about a tough day over a cup of tea.
Access to Australian Unity's mental health program Mindstep and an Employee Assistance Program that offers counselling and resources also play an important role in an industry where carers may regularly work with vulnerable people or need to cope with the deaths of long-time customers.
Such measures are significant, says Leona, as they help make a carer’s job more sustainable in the long term and lessen the risk of burnout. “You have to be able to switch off when you go home because sometimes you can take things with you,” she says.
This sort of training, support and connection can help make a demanding role more viable and fulfilling—something that's particularly vital given Australia’s need to recruit a vast number of carers in the years ahead. "We need to find ways to encourage people to consider it as a career pathway," emphasises Prue. "It really is one of the most wonderful professions."
Meet Leona
Leona started her journey with Australian Unity as a Care Worker, but has progressed to become our Branch Manager in Lithgow, New South Wales.
She supports a team of 12 and knows firsthand the benefit that structured support and training can provide.
Disclaimer: Information provided in this article is of a general nature. Australian Unity accepts no responsibility for the accuracy of any of the opinions, advice, representations or information contained in this publication. Readers should rely on their own advice and enquiries in making decisions affecting their own health, wellbeing or interest. Interviewee titles and employer are cited as at the time of interview and may have changed since publication.



