“You are not your cancer. You are not your condition. We are so much greater than the identities that we can fall into through this society.”—Dr Emily Tunks Macvean, founder of Embody Psychology.
Key points
- Physical and mental health is only one part of your overall wellbeing.
- Having a good relationship with your GP and health team is important.
- Joining a support group can make a huge difference.
For many of us, health and wellbeing are as interlinked as bacon and eggs, bread and butter, or avocado and vegemite.
But just as that last pairing can be somewhat questionable, so too is the idea of a clear-cut relationship between health and wellbeing. Why? Well, the state of our physical and mental health is only one of seven factors that contribute to our wellbeing, according to the Australian Unity Wellbeing Index, a 20-year study into the wellbeing and life satisfaction of Australians. And this knowledge can be a relief to those suffering from illness.
Dr Emily Tunks Macvean, founder of Embody Psychology, is a health psychologist who supports people with chronic pain, chronic conditions, life-threatening illnesses and mental health conditions. In her own work, Emily has noticed how a broader view of wellbeing can have a positive impact on a person’s life.
“Some of my clients are living with really difficult physical disorders or conditions, but have incredibly high wellbeing, because they’ve been able to separate themselves from just looking at the one narrow view of health as being physical,” she says. “It’s really exciting when you see these more holistic, more encompassing offerings of what it is to be human and how being healthy goes across all these different areas.”
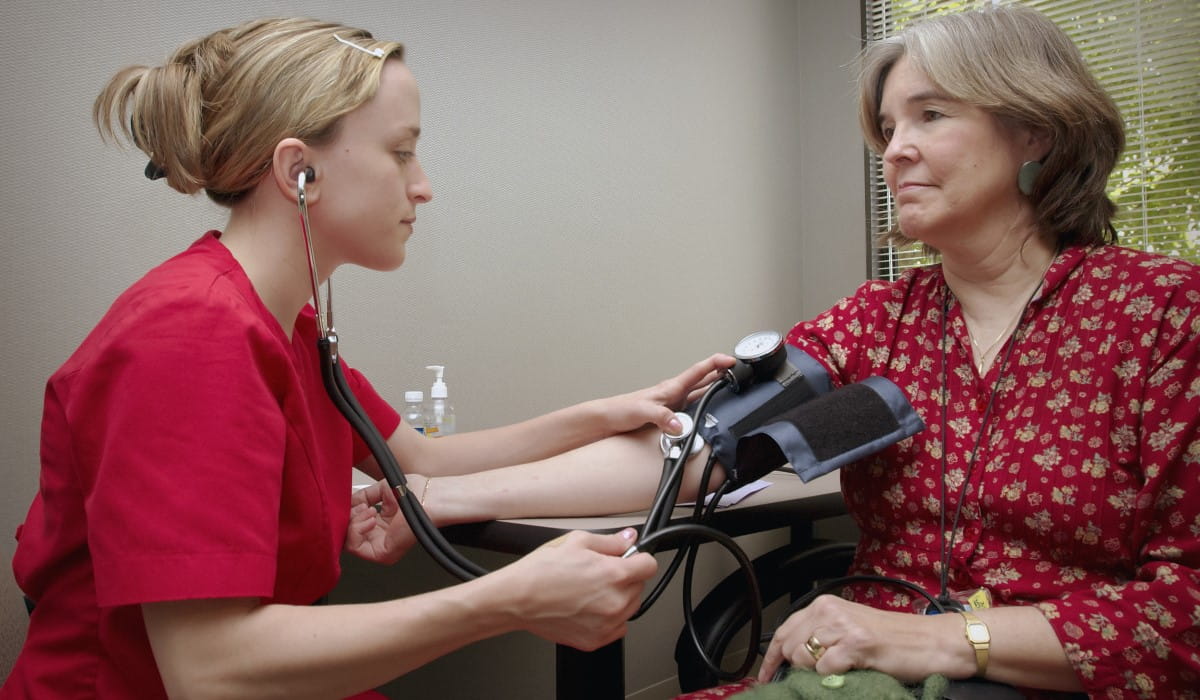
Getting some control back when it comes to health
For those suffering from physical and mental ill health, the first step to better wellbeing is finding credible information about what you’re experiencing, backed by a good relationship with your health team.
Whether it’s diabetes, cancer, heart disease or mental ill-health, there will be very clear and specific instructions to manage the symptoms, and advice to prevent deterioration and improve our lifestyle factors.
Findings in the Australian Unity Wellbeing Index shows that conditions that are well managed may have little impact on wellbeing. In the study, Deakin University researchers found that people with high blood pressure reported higher personal wellbeing scores than those with some other medical conditions, likely due to the fact that high blood pressure can be managed with medication and typically doesn’t restrict someone from taking part in everyday activities.
It also helps to plan for your future health. “Think about the future but don’t let it freak you out,” says Dr Sue Ferguson, a health psychologist and honorary associate lecturer in the Faculty of Medicine, Health and Human Sciences at Macquarie University.
“For instance, older adults with multiple chronic illnesses and some progression of disability might have to talk to their doctor about how long it’s likely to be before they need some help around the house or might need to go into care more permanently. Be aware of what's likely to happen and come up with long-term and short-term to-do lists.”
Redefining connections and purpose
The Australian Unity Wellbeing Index indicates that the effect of ill health on our wellbeing may also be able to be mitigated by factors such as good relationships and a sense of purpose, with a 2014 study showing that health satisfaction was less important to the overall wellbeing of people on dialysis than what they were achieving in life.
Emily also highlights the importance of relationships and a strong sense of community, explaining: “Some people need connection more than others—[and it varies according to] different personality types and social conditioning—but this connectedness helps protect physical and psychological health.”

This is why joining a support group can make a huge difference. “Whether it's related to your health condition or just your interest in snorkelling, it lessens that sense of loneliness or isolation,” says Emily. “Because that sense of loneliness is where I see the greatest suffering, connection is such a buffer.”
Emily also notes that reassessing your goals in light of your illness or condition is important. “Where I see people do better with their health is when they’re able to be flexible psychologically, not just physically,” she says.
She goes on to give an example of a surfer she worked with who suffered from an accident. “He had certain functional limitations and wasn’t able to surf again. Naturally, there’s a huge amount of adjustment and grief that has to be felt and experienced and not downplayed.
“But we came to a point where we were able to say, ‘This is a passion of yours. We'll have to change some of your previous goals, but how do we still get the essence of those goals in other ways?’ It requires being flexible. He went on to be a great stand-up paddleboarder.”
Sue has experienced this firsthand and has found ways to contribute to society within her capacity. “For me, I’ve found that being able to support other people takes my mind off my own issues,” she says. “I do several different volunteer tasks from my own home. When I'm having a really bad pain day, I can lie on my lounge and still volunteer. Finding that sense of meaning and purpose as your roles change is really important.”
Underpinning all of this is a point Emily makes: you are not your diagnosis. “You are not your cancer. You are not your condition. We are so much greater than the identities that we can fall into through this society.”
Emily continues: “When I’ve seen such incredible shifts in my clients, the sweet point is where there’s acceptance, flexibility and mindfulness skills. Sure, their pain level might not change, or it might come down a bit, yet their quality of life might be better than when they had their diagnosis because they know themselves better. They put in boundaries that protect their health. They know what brings them joy.”
Disclaimer: Information provided in this article is of a general nature. Australian Unity accepts no responsibility for the accuracy of any of the opinions, advice, representations or information contained in this publication. Readers should rely on their own advice and enquiries in making decisions affecting their own health, wellbeing or interest. Interviewee titles and employer are cited as at the time of interview and may have changed since publication.


